By Rainey Horwitz, MS
Vibrators are gaining attention among physicians for their therapeutic roles in medicine. Despite the long medical history of therapeutic pelvic massage around the world, personal massagers like vibrators are just entering mainstream conversation and gaining recognition as a pelvic health therapy by Western medicine. This is likely connected to sexual stigma and taboo surrounding imagery and discussion of vibrators. Vibrators were initially used in medical offices during the industrial revolution of the early 1900s when electrical power entered private establishment. Vibration was claimed to be a treatment for gastrointestinal and lymphatic issues, as well as supposed energetic “rejuvenation” remedies. Following their appearance in pornography in the 1920s, vibrators became tied to sexual deviancy and were no longer recognized for their potential therapeutic roles (Horwitz, 2020).
| Shapes | Example | Description | Uses | |||||
| Bullet |
|
Small, tapered finger shape, often use batteries | External stimulation of glans clitoris. Most simple design and best suited for first time users. Easy to travel with. | |||||
| Palm |
|
Fits in palm, variety of pebble-like shapes | External stimulation of glans clitoris. Small, easy to place and utilize for partnered sex. | |||||
| Finger |  |
Vibrating component attached to a ring that is worn on finger | External stimulation of glans clitoris, nipples. Small, easy to place, and incorporate in partnered sex. | |||||
| Dildo |
|
Phallic in shape, varying dimensions to accomodate different anatomy | Internal cervix, clitorourethral complex, vaginal stimulation | |||||
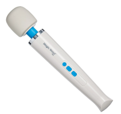
| Wand |
|
Longer handheld device with a flexible, high-powered, vibrating head. | External stimulation of glans clitoris. Highest intensity vibration. Ideal for those requiring powerful stimulation (aging, anorgasmia). Somewhat bulky with rechargeable and wall-outlet options. Also useful as a back massager. | |||||
| U Type |
|
C-shaped with internal and external component | External stimulation of glans clitoris with internal stimulation of clitorourethral complex via small insert | |||||
| Rabbit |
|
Phallic/dlido shaped internal component with small external component | External stimulation of glans clitoris with internal stimulation of clitorourethral complex via large, often dildo-like insert | |||||
| Anal plug |
|
Body safe with flared base, can have design for prostate stimulation | Internal anal/prostate stimulation | |||||
| Ring |
|
Wearable penile constriction ring with vibrating component attached | Constriction ring assists with prolongation of erection and vibrating component can stimulate external glans clitoris in positions where partners are facing | |||||
| Stroker |
|
Vibrating sleeve-like device for penile stimulation | Useful in penile rehab, recovery of sensation, can be used while flacid or erect | |||||
| Remote control |
|
Often have insertable internal component with remote control | Partnered experimentation. Ideal for limited use of hands | |||||
| Pad |
|
Pad with vibrating component intended for sitting on/grinding | Ideal for limited use of hands |
In the modern era, physician researchers have started exploring practical roles for vibrators in pelvic health. While limited data exists at this time regarding the health benefits of local genital vibration, a systematic review published early this year by a group of urogynecology researchers found available evidence to support an underutilized therapeutic role for vibrators in treating several pelvic health concerns. Specifically, evidence supports the use of vibrators as an accepted modality to aid in female sexual function, improve pelvic floor muscle function, and facilitate the treatment of vulvar pain (Dubinskaya, 2023). While this study examined the role of vibrators among female patients, vibrators can demonstrate health benefits in patients regardless of gender and genital anatomy.
In terms of sexual function, vibrators improve arousal by promoting local vasodilation and blood flow to the pelvic floor muscles. Vibrator use decreases orgasm latency and facilitates multiple orgasms. In a study surrounding a holistic approach to treating anorgasmia, among the 500 women who had anorgasmia for an average of 12 years, 93% (n=465) were able to experience orgasm with the use of a high intensity vibrator (Struck, 208).
Vibrators are also an underutilized modality in pelvic rehabilitation. Many people with vulvas live with conditions like pelvic floor dysfunction and subsequent stress urinary incontinence, with few non-surgical treatments available. Local vibration can be applied to the pelvic region to train pelvic floor muscles by promoting involuntary contractions, an especially useful characteristic for patients who lack voluntary control of their pelvic floor or cannot perform Kegel exercises. Improvements in pelvic floor tone were shown to decrease pad usage and decrease perceived leak symptoms following intervention with a pelvic vibrator. Specifically, vibration in combination with biofeedback appears to be a promising tool to improve pelvic floor tone.
Lastly, vulvar vibration therapy (VVT) has been described in one study as a well-tolerated treatment for chronic vulvar pain. Conceptually, the therapeutic role of vibrators in these patients is based on the antinociceptive properties of vibration and temporary desensitization (Zolnoun, 2008).
Sexual function and the role of vibrators is not typically discussed in medical training curriculum, so many physicians may feel ill equipped to provide vibrator/sex tool recommendations to their patients. Vibrators vary by speed, shape, and intensity of vibration. Few studies have teased out the functional characteristics of commercial vibrators, however one study noted that intensity can be considered among aging women and women with urinary incontinence, multiple sclerosis, and/or sexual dysfunction potentially requiring higher intensity vibration (Connell, 2004)(Gruenwald, 2007).
Physicians can aid patients by promoting conversation about the use of vibrators as a health aid and preventative health measure for preservation of pelvic tone. Normalizing conversations about vibrators in the physician's office may help decrease patient anxiety and increase patient trust of this well tolerated, relatively inexpensive intervention historically tied in unnecessary shame. Physicians can provide resources in the form of affordable, body safe vibrator recommendations and assist patients in selecting the most appropriate model and functions for their anatomy and concerns. For example, a patient recovering from a gender-affirming vulvaplasty with a canal may best be suited with an external clitoral vibrator that fits in the palm. Later when neo-vaginal tissues have healed, dilation of the new canal can be augmented with a vibrator with a narrow penetrative portion. Encouraging use of lubricant and safe cleaning and storage of sex tools is also an important consideration to discuss with patients.
You may also be interested in...
Other Popular Articles

What Is the Average Penis Size?
If you have ever wondered how your penis compares to others in terms of size, you are not alone. Many men are curious to know how their penises stack up compared to the average. Unfortunately, general curiosity can sometimes give way to full-on obsession and anxiety about penis size. This can be an unhealthy and often unnecessary fixation, especially because most men who think their penises are too small have perfectly normal-sized penises.

What Is Sensate Focus and How Does It Work?
Sensate focus is a technique used to improve intimacy and communication between partners around sex, reduce sexual performance anxiety, and shift away from ingrained, goal-oriented sexual patterns that may not be serving a couple.

What Is Jelqing, and Does It Actually Work?
The term “jelqing” refers to a set of penis stretching exercises that some believe can make the penis bigger. Although the practice has gained attention and popularity in blogs and internet forums in recent years, there is no scientific evidence that it is an effective way to permanently increase the size of one’s penis. In fact, in some cases, jelqing may actually cause damage to the penis, so it is a good idea to get all the facts before setting off to try it.

Can Sex Reduce Menstrual Cramps?
The SMSNA periodically receives and publishes ‘guest editorials.’ The current article was submitted by Mia Barnes, a freelance writer and researcher who specializes in women's health, wellness, and healthy living. She is the Founder and Editor-in-Chief of Body+Mind Magazine.
Having sex while you experience menstrual cramps is healthy and can provide significant benefits. While it might not be the first activity that comes to mind when your PMS or period cramping begins, many people enjoy sex to reduce menstrual cramps, experience increased pleasure and benefit from other advantages. Learn more about having sex while menstrual cramps are happening and how it can help your body.

How Long Does It Take the Average Man to Ejaculate?
On average, it takes a man between 5 to 7 minutes to orgasm and ejaculate during sexual intercourse.

Can Sex Throw off Your Vaginal pH Balance?
The SMSNA periodically receives and publishes ‘guest editorials.’ The current article was submitted by Mia Barnes, a freelance writer and researcher who specializes in women's health, wellness, and healthy living. She is the Founder and Editor-in-Chief of Body+Mind Magazine.
Your vagina is a pretty powerful organ. It is a pathway for menstrual blood and babies. It also is a main player in sexual intercourse. You might hear about your vagina’s pH and worry that yours is at risk. Here’s what to know about vaginal pH, including the impacts sex could have.
You are prohibited from using or uploading content you accessed through this website into external applications, bots, software, or websites, including those using artificial intelligence technologies and infrastructure, including deep learning, machine learning and large language models and generative AI.