Did You Know?
Stress urinary incontinence and erectile dysfunction (ED) are common side effects after any level of prostate cancer treatment, including radical prostatectomy and radiation therapy for prostate cancer. While many patients prefer to treat bothersome incontinence first, over ED, this is no longer a polarizing choice, and there are effective surgical management solutions for both.
GLP-1 medications have become widely discussed in recent years. It may feel like every time you turn on your favorite show on streaming, there are a thousand ads about the next semaglutide or another injection or pill available for weight loss. But what is a GLP-1, and how could it affect your sexual health?
Erectile dysfunction (ED) is common and occurs in men (around 30 million in the U.S.) resulting in issues getting and keeping an erection. ED can occur because of physical, hormonal, or psychological reasons, which means there are many ways to treat it. (Rojanasarot et al., 2023)
Sickle cell disease (SCD) is a condition people are born with that changes the way their body makes red blood cells. Instead of being donut-shaped and squishy, they form into a C-shape (sickled) and are stiffer and tend to clump together, which can make it harder for oxygen to travel through the bloodstream.
Apomorphine is a medication typically used for treating “off” episodes of Parkinson’s disease. It works by activating dopamine receptors in the brain, helping to replace or mimic the effects of natural dopamine. Since dopamine plays a role in sexual arousal, apomorphine could potentially influence one’s desire and libido, as well as help with stimulating erections.
Endometriosis is a chronic, estrogen-dependent condition affecting around 10-20% of women at reproductive age. It occurs when endometrial tissue (uterine lining) implants itself outside the uterus. Typically, it implants itself in areas that would still be along the reproductive system, such as the fallopian tubes and ovaries, but sometimes this tissue may travel to the urethra, bowel and intestines, or further. Symptoms of endometriosis depend on the severity of excess tissue growth:
Globally, around 44% of pregnancies are unintended. Of these, about two-thirds were due to not using contraception, or using unreliable methods (pull-out, etc.). This tends to place women at risk for harmful procedures that may have otherwise been avoided. The issue lies with the burden of prevention primarily being placed on women, usually in the form of hormonal birth control options that may not be the best for every woman.
Currently, over 80% of Americans consume caffeine daily (around 200 mg per day), with the majority of caffeine coming from coffee. Outside of coffee, other major sources of caffeine include soda/pop and energy or sports drinks. But will your next caramel macchiato, Celsius, or pre-workout scoop tank your libido (sexual desire)?
Polycystic ovary syndrome (PCOS) is known as one of the most common hormonal disorders in females of reproductive age worldwide, with prevalence ranging from 5-26% of women.
You may have had a sexual experience where you ejaculated and thought, “Hmmmm, that doesn’t look right, am I okay right now?” You are not alone. There are plenty of people with penises that have similar experiences. However, it’s important to keep track of what your normal ejaculate looks like, so you can keep an eye out for any underlying condition that can be identified in part by the look and texture of semen. Did you know that some ejaculate is more normal than others?
Many women may have heard from mother figures or other women in their lifetime that continuing to use the same tampon past 6 hours will cause toxic shock syndrome (TSS), perhaps without ever truly knowing what it is, only knowing that it does not sound good. Meanwhile, other women throw caution to the wind, often continuing to use the same tampon for a whole day with no consequences. Did you know there’s more to TSS than time with a tampon in?
Scrotal pain could be the result of a variety of conditions and is a common complaint in emergency rooms and doctor’s offices. But did you know that scrotal pain could be the result of a potentially serious condition?
Fetishes, along with fetishism, have a variety of definitions depending on the severity of the individual’s obsession level. Fetishes are considered any recurring and intense sexual fantasy involving an object or nonsexual body part. For example, one could have a fetish for the feeling of lace, or for feet in general. While many fetishes are seen more as a sexual preference, they may become problematic when this sexual preference persists for longer than 6 months and causes distress for the individual, which is known as paraphilia. Most existing research (while there is very little) understands that fetishism to this degree is primarily encountered by men, though women can also have fetishes.
Cannabis, also known as marijuana, is a plant which has been used for centuries in traditional medicine practices and outside of those for purposes relating to spirituality and recreation. Within cannabis, there are over 400 different compounds. Of these, over 100 belong to the class known as cannabinoids, which are responsible for their well-known calming and psychotropic effects. The most common cannabinoids sold commercially are Delta 9-THC (THC), and cannabidiol (CBD), the latter of which offers more calming effects.
Aphrodisiacs, named after the Greek goddess Aphrodite, are known to most as specific foods, herbs, or other consumable substances that supposedly help with libido (sex drive) and sexual functioning. Proclaimed aphrodisiacs may have some properties that support the human processes involved in sexual activity, such as natural chemicals that help increase libido, testosterone levels, and endothelial function (the regulation of blood flow). They have also been thought to improve sexual desire, fertility, and sexual pleasure. However, there are also several foods or supplements that became known as aphrodisiacs simply by way of marketing.
Foreplay refers to the emotionally and physically intimate behaviors leading up to sexual intercourse: the gateway to sexual excitement and desire. It can consist of anything from flirting and kissing, to grinding and massages, to removing clothes and roleplaying. While some may not see the importance, there are a lot of very good reasons to engage in foreplay. Everyone needs some sort of psychological or emotional stimulation in order to become aroused. According to the sexual response cycle, the “desire” phase is what may be initiated by foreplay and is imperative to sexual activity. In this phase, muscle and sexual tension increases, the heart rate becomes faster leading to increased blood flow in the genitals – this causes both penile and clitoral erection – and the vagina may begin to self-lubricate while the penis may begin to leak pre-ejaculate.
A sex journal, or sex diary, is exactly what it sounds like: a place you can go to write specifically about sexual activity, encounters, sensations and more. In the past few years, there has been an uptick in interest about sex journals and the influences they can have on a person’s sex life – or communication with a partner. Some wellness websites even sell guided sex journals, with the intention that they will help someone activate their best sexual self.
Painful ejaculation, also referred to as dysorgasmia or orgasmalgia, is exactly what it says, pain in the genitals or groin area right before, during or after ejaculation for a variable amount of time – from just a few seconds and up to two days. The sensation can range from a dull ache to unbearable pain and can be localized to the penis (including the urethra), testes, perineum, or further into the lower abdomen or rectum.
A Loop Electrosurgical Excision Procedure (LEEP) is a common treatment used to remove abnormal cells from the cervix, often following an abnormal Pap smear. This procedure is typically recommended when a woman has cervical dysplasia, which refers to the presence of precancerous cells that could develop into cervical cancer if left untreated.
Acupuncture and herbal remedies have been used for centuries in traditional medicine systems like Traditional Chinese Medicine (TCM) and Ayurveda. With increasing interest in holistic approaches to health, many people wonder if these practices can enhance their sex life. Here’s a look at what scientific research says about their potential effects.
Sexual activity is often seen as a pleasurable and intimate experience, but like any physical activity, it can occasionally lead to injuries. While many injuries are minor and temporary, some require medical attention. Understanding common sex-related injuries can help individuals prevent them and maintain healthy sexual experiences.
A healthy, active sex life is an important part of overall well-being for many people. Just as we strive to extend our lifespan with good health habits, it’s possible to expand our sexspan – the ability to maintain a satisfying sex life well into older age. By focusing on physical, emotional, and relational health, you can take steps now to support sexual wellness for the long term.
Obstructive sleep apnea (OSA) is a common sleep disorder characterized by repeated interruptions in breathing during sleep due to airway blockage. Affecting about 5 – 20% of adults, OSA has been linked to poor sleep quality, fatigue, and various health issues, including sexual dysfunction. Studies have examined connections between OSA and both male and female sexual dysfunction, suggesting that untreated OSA may contribute to reduced sexual health and satisfaction.
Choking or strangulation during sexual activities is something that has garnered significant attention recently. New research has sparked a rise in awareness of this practice, particularly among teenagers and young adults, with statistics revealing that 64% of women reported having experienced choking during sex. Despite the thrill that some individuals might associate with this behavior, the health risks associated with choking are serious and often overlooked.
Breast cancer treatment often includes hormone therapies, which can be highly effective in reducing cancer recurrence and improving survival rates. However, these therapies can also impact a woman’s sexual health and overall quality of life. Many women experience changes in libido, vaginal health, and sexual function during and after treatment, which can be difficult to navigate emotionally and physically.
Inflatable penile prosthesis (IPP) surgery is a common treatment option for men with erectile dysfunction (ED) who haven’t found success with other treatments like medication or injections, or who desire a permanent solution for their ED. It involves surgically inserting a penile implant into the penis that allows an individual to get an erection on demand by inflating the implant when necessary.
The SMSNA periodically receives and publishes ‘guest editorials.’ The current article was submitted by Mia Barnes, a freelance writer and researcher who specializes in women's health, wellness, and healthy living. She is the Founder and Editor-in-Chief of Body+Mind Magazine.
Living your life with a partner is a daily learning experience. You’re always picking up on their emotional cues, but people sometimes forget to develop their awareness of sexual arousal cues. Learn more about erotic intelligence to understand if you have it and how to develop it further.
Anabolic steroids, also known as anabolic-androgenic steroids (AAS), are synthetic substances that are similar to the male hormone testosterone. They are used medically to treat hormonal issues but can be misused by athletes and bodybuilders to enhance muscle growth and performance. Steroids can improve a person’s physical performance and appearance, but they come with significant health risks, particularly concerning sexual health.
The SMSNA periodically receives and publishes ‘guest editorials.’ The current article was submitted by Mia Barnes, a freelance writer and researcher who specializes in women's health, wellness, and healthy living. She is the Founder and Editor-in-Chief of Body+Mind Magazine.
Porn consumption is linked to various negative effects, including poor self-image. It can easily foster feelings of inadequacy and resentment for men and women. Discover the link between porn and body image and some signs of negative self-perception to look out for.
Migraines are debilitating headaches that affect approximately 14% of the global population annually. These intense headaches, often accompanied by symptoms such as nausea, sensitivity to light and sound, and chills, can significantly impact an individual’s quality of life. Interestingly, the relationship between migraines and sexual activity is complex, with sex potentially acting as both a remedy and a trigger for migraines. This article explores the dual role of sex in the context of migraines, highlighting research findings and expert insights.
Mental health conditions such as depression, anxiety, and bipolar disorder are prevalent worldwide, and medications to treat these conditions can be life-changing for many individuals. However, these medications often come with side effects, some of which can impact sexual health of both men and women. Understanding these effects is the first step for patients and healthcare providers to managing and mitigating them effectively.
Body image plays a significant role in shaping an individual’s self-esteem and overall sense of self-assurance. However, its impact extends beyond mere appearance—it deeply influences one’s sexual confidence and satisfaction within intimate relationships. This article explores the intricate relationship between body image and sexual experiences, shedding light on the ways in which body perception can either enhance or hinder sexual confidence and satisfaction.
Colposcopy is a medical procedure that is often recommended for individuals who have abnormal cervical screening results. It is an important step in diagnosing and managing conditions such as cervical dysplasia (changes in the cervical cells) or cervical cancer. Understanding what to expect during a colposcopy can help alleviate anxiety and pave the way for a smoother experience.
May is National Masturbation Month, and as such, it is time to acknowledge the benefits of an activity that is often shrouded in secrecy and taboo. While discussions about masturbation may evoke discomfort for some, it is important to recognize that it is a perfectly natural and healthy aspect of human sexuality. Beyond the pleasure it provides, masturbation offers numerous health benefits that can contribute to a person’s overall well-being. For those who may feel ashamed or hesitant to explore this topic, understanding the science behind the benefits of masturbation can offer reassurance and empowerment.
April is Testicular Cancer Awareness Month, aimed at spreading awareness about the disease and encouraging men to prioritize their health through regular screenings and education. Testicular cancer is a less common form of cancer, but understanding its risk factors and taking preventative measures can help with early detection and successful treatment. The following are the various risk factors associated with testicular cancer as well as ways to lower one’s risk.
Embarking on a journey of sobriety is a significant step towards physical, mental, and emotional well-being. While the focus is often placed on the cessation of substance use itself, it may also be helpful to acknowledge the potential impact of sobriety on various aspects of life, including sexual health. Transitioning to a sober lifestyle can indeed bring about changes in sexual behavior, desires, and experiences. Understanding these changes and navigating them with proper guidance and support is essential for individuals embracing sobriety.
By Rainey Horwitz, MD, MS
Penile constriction rings are devices designed to be placed around the base of the penis to aid in maintaining an erection by restricting the outflow of blood. There are several reasons people with a penis might be interested in exploring the use of rings during sex. Many wearers appreciate that penile constriction rings/bands can aid in enhancing erectile function by gently compressing the veins that drain blood penis, causing the corpora to retain blood and remain firmer for a prolonged period of time. Difficulty maintaining rigidity can be a source of distress for people with a penis, so penile rings offer a safe option to try before utilizing erectile dysfunction medications. Some rings are specifically designed to be used in conjunction with vacuum erection devices (VEDs) to treat erectile dysfunction by maintaining corporal blood flow with negative pressure. Penile rings and VEDs are examples of conservative approaches to treating erectile dysfunction and can also be useful augmentations in optimizing erectile function prior to and following urologic surgery.
The realm of birth control is vast and diverse, offering individuals the ability to make informed choices about their reproductive health. Understanding the various types of birth control methods and how they work is crucial for anyone seeking to take control of their family planning. This article will explore different types of birth control and explain the mechanisms behind each method.
Bumps on the genitals can be a source of concern and discomfort for individuals, prompting questions about their causes and potential implications. It is important to recognize that various factors can contribute to the development of genital bumps, and understanding these causes is essential for proper diagnosis and effective management.
Feminine hygiene is a topic of paramount importance for women’s health and well-being. Over-the-counter (OTC) feminine hygiene products are widely available and commonly used to address various intimate health concerns. However, a critical question that often arises is whether these products are safe or beneficial for use. This following is a list of commonly sold feminine hygiene products along with information on their potential risks and/or benefits.
The SMSNA periodically receives and publishes ‘guest editorials.’ The current article was submitted by Mia Barnes, a freelance writer and researcher who specializes in women's health, wellness, and healthy living. She is the Founder and Editor-in-Chief of Body+Mind Magazine.
You might panic if you notice a fishy discharge down there. While your symptoms may spur worry, the problem could be a readily treatable and common condition known as bacterial vaginosis.
Human immunodeficiency virus (HIV) and acquired immunodeficiency syndrome (AIDS) have been a global health concern for decades, with misinformation and myths often contributing to the stigma surrounding these conditions. Despite extensive efforts to educate the public, numerous myths persist. This article aims to debunk some of the most common misconceptions about HIV/AIDS, providing accurate information to promote understanding and reduce stigma.
Premenstrual syndrome (PMS) is a common condition that affects many individuals with uteruses during their menstrual cycle. PMS is known for its physical symptoms such as bloating, breast tenderness, headaches, and cramps, as well as its emotional symptoms including mood swings, irritability, anxiety, and feelings of sadness. Nevertheless, its impact on sexual well-being is often overlooked.
The SMSNA periodically receives and publishes ‘guest editorials.’ The current article was submitted by Mia Barnes, a freelance writer and researcher who specializes in women's health, wellness, and healthy living. She is the Founder and Editor-in-Chief of Body+Mind Magazine.
Your vagina is a pretty powerful organ. It is a pathway for menstrual blood and babies. It also is a main player in sexual intercourse. You might hear about your vagina’s pH and worry that yours is at risk. Here’s what to know about vaginal pH, including the impacts sex could have.
Peyronie’s disease (PD) occurs when scar tissue (plaque) under the skin of the penis causes it to bend or change shape when it becomes erect. Often, this condition is associated with a loss of penile length or girth. It is considered to be a sexual dysfunction because PD may make it difficult or impossible for an individual to have sex. While the exact cause of PD is unknown and may vary from person to person, it can be related to an injury or a connective tissue disorder.
The SMSNA periodically receives and publishes ‘guest editorials.’ The current article was submitted by Mia Barnes, a freelance writer and researcher who specializes in women's health, wellness, and healthy living. She is the Founder and Editor-in-Chief of Body+Mind Magazine.
Practicing safe sex is essential. Everyone deserves protection against unwanted pregnancies, but making informed decisions without learning if a contraceptive method is effective is challenging. Discover if the pull-out method actually works and whether you should switch to an alternative form of contraceptives.
The SMSNA periodically receives and publishes ‘guest editorials.’ The current article was submitted by Mia Barnes, a freelance writer and researcher who specializes in women's health, wellness, and healthy living. She is the Founder and Editor-in-Chief of Body+Mind Magazine.
Your hormones can influence things large and small, including something as crucial as your mood. When your body doesn't produce enough of one, it can throw things off drastically. You may experience side effects ranging from depression to unexplained weight loss or weight gain. Knowing how your sex hormones can regulate your libido can help you better understand yourself overall.
Watching pornography (porn) has become an increasingly common phenomenon that occurs at a progressively younger age, given the availability, anonymity, and accessibility of porn on the internet. Viewing pornography is common and normal, even though some individuals may feel concerned about the frequency at which they watch porn.
Micropenis is a medical condition in which an individual has an atypically small penis. Although a universal definition for micropenis has not been agreed upon, one proposed definition is a penis of an adult man that is 9.3 cm or 3.66 inches or less when stretched (while flaccid). The average penis length for an adult man is 13.24 cm or 5.21 inches when stretched.
The SMSNA periodically receives and publishes ‘guest editorials.’ The current article was submitted by Mia Barnes, a freelance writer and researcher who specializes in women's health, wellness, and healthy living. She is the Founder and Editor-in-Chief of Body+Mind Magazine.
Breastfeeding is a beautiful way to nourish your child and strengthen the mother-baby bond. It can also affect your sex life and sexuality. Prior to giving birth, breasts were an erogenous zone meant for your and your partner’s pleasure. Now, they have more than one function, which can feel confusing. In addition, surging hormones from breastfeeding can change how a woman’s body reacts to sexual stimulation.
By Rainey Horwitz, MS
Vibrators are gaining attention among physicians for their therapeutic roles in medicine. Despite the long medical history of therapeutic pelvic massage around the world, personal massagers like vibrators are just entering mainstream conversation and gaining recognition as a pelvic health therapy by Western medicine. This is likely connected to sexual stigma and taboo surrounding imagery and discussion of vibrators. Vibrators were initially used in medical offices during the industrial revolution of the early 1900s when electrical power entered private establishment. Vibration was claimed to be a treatment for gastrointestinal and lymphatic issues, as well as supposed energetic “rejuvenation” remedies. Following their appearance in pornography in the 1920s, vibrators became tied to sexual deviancy and were no longer recognized for their potential therapeutic roles (Horwitz, 2020).
Sex toys and tools such as vibrators, dildos, vaginal dilators, anal toys, penis rings, and penis sleeves can enhance a solitary or partnered sexual experience. However, it is important to use them safely. By using sex toys responsibly and keeping them clean, you can avoid passing on sexually transmitted infections (STIs) and/or blood-borne infections (from sex toys that may create small tears in the skin and draw blood).
The SMSNA periodically receives and publishes ‘guest editorials.’ The current article was submitted by Mia Barnes, a freelance writer and researcher who specializes in women's health, wellness, and healthy living. She is the Founder and Editor-in-Chief of Body+Mind Magazine.
Many women experience ebbs and flows in their libidos throughout their pregnancies. While one woman may have an increased sex drive, another can lack desire altogether. An increased or decreased libido is normal and can vary by the woman and even by pregnancy. Some women experience a high sex drive in their first pregnancy and a low one in their second. Here are some reasons why.
Obsessive compulsive disorder (OCD) is a chronic mental health condition that involves recurring unwanted thoughts or impulses (known as obsessions) that lead to repetitive behaviors (compulsions). These obsessions and compulsions can interfere with a person’s day-to-day life and may cause relationship problems, occupational issues, and significant emotional distress.
Provoked vestibulodynia (PVD) is a condition that can affect people who have vulvas, causing painful sex. It is a form of vulvodynia (pain in the vulva, or external female genitalia) that is characterized by pain with touch or pressure on the vulvar vestibule, which is the skin by the entrance to the urethra and vaginal opening.
The SMSNA periodically receives and publishes ‘guest editorials.’ The current article was submitted by Mia Barnes, a freelance writer and researcher who specializes in women's health, wellness, and healthy living. She is the Founder and Editor-in-Chief of Body+Mind Magazine.
Pain during sex, or dyspareunia, is often treatable and very common among women. You could experience pain during intercourse, and you shouldn’t be embarrassed or afraid to discuss it with your doctor. It may feel like a burning sensation or a more profound physical pain. Some common causes of discomfort during penetration can be dryness, irritation, injury or inflammation. Here are some other reasons you could experience pain during sex.
Movember is an annual awareness-raising event that occurs every November. It involves growing a moustache throughout the month to bring attention to men’s health issues including prostate cancer, testicular cancer, and men’s suicide. The name “Movember” is a combination of the words “moustache” and “November.” Here is some information on the important men’s health issues that are addressed in Movember.
According to a recent retrospective cohort study, low testosterone levels in men may increase their risk of hospitalization for COVID-19. Conversely, normal testosterone levels in men, (whether due to the body’s natural production of testosterone or testosterone therapy,) may be protective against severe cases of COVID-19.
The pelvic floor is a group of muscles that holds the pelvic organs in place. A strong pelvic floor is associated with good sexual outcomes. People may encounter sexual health issues if their pelvic floor muscles become too weak, including pelvic organ prolapse or urinary or fecal incontinence during sex. On the other hand, sexual problems can also arise when the pelvic floor muscles are too tight.
A stim patch is a small (disposable) electrical device that can be worn on the perineum (the area between the anus and the scrotum) to delay premature ejaculation. It works by delivering electrical stimulation to the body that may help men contract the muscles of their pelvic floor and, in doing so, postpone ejaculation during sexual activity.
The P-Shot, also known as a platelet-rich plasma (PRP) injection, is being tested as an experimental therapy for erectile dysfunction (ED). It involves taking a sample of the patient’s blood, using a centrifuge to separate out the PRP from the other components of blood (i.e., red blood cells and platelet-poor plasma), and injecting the PRP into the penis to promote the growth of penile tissues.
Cybersex is any type of sexual activity that occurs virtually between two or more individuals including sexting, sharing sexual images or videos with a partner, webcam sex, and chatroom sex. Although some cybersex experiences include visual elements such as photos or video, other cybersex activities involve describing sexual fantasies or scenarios in written or spoken words. In most cases, cybersex involves real-life masturbation by one or all participants.
Although it is rare, penile fracture is possible when a man experiences trauma to his erect penis, sometimes during rough sexual intercourse. Since there are no bones in the penis, penile fracture is different from other types of fractures. It occurs when the corpora cavernosa (two columns of spongy tissue in the penis that fill with blood during an erection) are damaged due to a sudden blow or a situation in which the erect penis is bent forcefully.
Phosphodiesterase type 5 inhibitors (PDE5i) are oral medications used to treat erectile dysfunction (ED) such as Viagra, Cialis, and Levitra. They are one of the most frequently prescribed medications in the U.S., and in 2020, an estimated 20 million monthly PDE5i prescriptions were filled within the country.
Some studies have suggested there may be a relationship between cycling and erectile dysfunction (ED) in men. However, before you panic and sell your bicycle, take into consideration that, at this time, the evidence on the topic is still limited and conflicting. The potential association between cycling and ED is likely more nuanced than one might expect. What’s more, there may be ways for cyclists to protect themselves against ED. Although this article is not a substitute for advice from a medical professional, it may help clarify some points regarding cycling and ED.
Pornography use has become more prevalent in recent years due to the ease of access of readily available free content on porn streaming websites. By some estimates, over half of all men and one-third of all women watch porn at least once a year. Nevertheless, it remains somewhat controversial, and sexual medicine experts have debated the possible role of frequent porn viewing in sexual dysfunction, relationship problems, and sexual dissatisfaction.
The microorganisms that inhabit the vagina are known as the vaginal flora or microbiome. Maintaining a healthy vaginal microbiome is important because it can help prevent infection, support fertility, and improve a woman’s quality of life. Unfortunately, not all products and behaviors promoted as “feminine hygiene” have a beneficial effect on the vaginal flora. The following are facts on vaginal health and feminine hygiene to help you sort through some of the most common misconceptions.
Orgasm is part of the sexual response cycle for both men and women. It is the point during sexual response in which a person’s blood pressure, heart rate, and breathing reach their maximum rate, along with transient peak sensations of intense pleasure, creating an altered state of consciousness. Typically, orgasm is described as a sudden release of sexual tension accompanied by involuntary muscle contractions, especially those in the pelvic region and around the sexual organs. Women experience contractions in the uterus and vagina, and men have contractions in the muscles at the base of the penis, usually resulting in ejaculation.
One of the most frequently asked questions among people who are considering getting a penile prosthesis (implant) to treat erectile dysfunction (ED) is: How will my partner feel about it? Fortunately, research indicates that partners’ responses to penile implants are generally positive and partner satisfaction rates are high.
A penile prothesis, or penile implant, is a device that is surgically inserted into the penis to treat erectile dysfunction (ED). Getting a penile implant is a big decision, but one that can restore an individual’s sexual function and, in many cases, improve his sexual quality of life.
The term “jelqing” refers to a set of penis stretching exercises that some believe can make the penis bigger. Although the practice has gained attention and popularity in blogs and internet forums in recent years, there is no scientific evidence that it is an effective way to permanently increase the size of one’s penis. In fact, in some cases, jelqing may actually cause damage to the penis, so it is a good idea to get all the facts before setting off to try it.
You may have heard references to “being sex-positive” or “the sex-positivity movement” in popular culture. Various celebrities have brought attention to this movement by speaking out about their beliefs and personal experiences regarding sexuality, sexual health, body positivity, “slut-shaming,” and sexual assault.
Painful intercourse, or dyspareunia, can be a frustrating, sometimes alienating problem. Many people consider sex to be a private matter and may be reluctant to talk about sexual pain or dysfunction with their health care providers. Nevertheless, because dyspareunia can be caused by injury, an underlying medical condition, or psychological reasons, it is a good idea to consult a health care professional if you experience frequent or long-term pain during intercourse. In the meantime, the following guide may provide a good starting point for determining why sex hurts.*
If you have ever wondered how your penis compares to others in terms of size, you are not alone. Many men are curious to know how their penises stack up compared to the average. Unfortunately, general curiosity can sometimes give way to full-on obsession and anxiety about penis size. This can be an unhealthy and often unnecessary fixation, especially because most men who think their penises are too small have perfectly normal-sized penises.
The results of a 2019 clinical trial of 1,000 European men with erectile dysfunction (ED) have led people to wonder: could a non-medicated topical gel really help men get erections? Unfortunately, the answer is probably, ‘no.’
Outercourse is a word used to describe sexual activities that do not involve penile-vaginal intercourse. It is a highly subjective term that is open to interpretation, so couples who choose to engage in outercourse should make sure that they are on the same page about which activities they want to include in (or exclude from) their sexual experiences. The following guide on outercourse can help you wrap your head around the concept.
Pelvic organ prolapse (POP) is a type of pelvic floor disorder that can cause painful and unpleasant symptoms for women, including dyspareunia, which is painful sex. It is estimated that about one-third of all women experience a pelvic floor disorder at some point in their lives, ranging from urinary or fecal incontinence (leaking of urine or stool, respectively) to POP. Here are the facts on pelvic organ prolapse.
Nothing can put a damper on an amorous mood faster than a case of alcohol-related erectile dysfunction (ED), also known in more vulgar terms as “whiskey dick.” While you and your partner may be excited to parlay your margarita buzz into an evening of sex, there could be times when your penis won’t rise to the occasion.
Perhaps you have heard the term “blue balls” used to describe sexual frustration in people with male genitals. Still, you may wonder, what exactly is “blue ball” syndrome? Does it really exist? If so, why does it happen? The following is a comprehensive guide on all you need to know about “blue balls.”
Prostate cancer survivors and their partners often face long-term sexual problems, especially erectile dysfunction (ED). Medical treatments can be effective, but some experts think adding other therapeutic approaches like mindfulness and acceptance may help even more.
Topical testosterone, which can be applied directly to the skin, is a convenient way for men with hypogonadism to undergo testosterone replacement therapy.
However, men should use it cautiously and keep these key points in mind:
Men with certain types of hypogonadism (low testosterone) can now administer their own testosterone injections at home, bringing their levels of this hormone into normal ranges.
Xyosted, which delivers testosterone therapy in a special one-use device, was approved by the U.S. Food and Drug Administration (FDA) in October 2018.
Sexual function can be difficult after breast cancer treatment. (Learn more.) Many women feel little desire for sex or have trouble becoming lubricated enough for comfortable intercourse. They might have more trouble reaching orgasm than they did before having cancer. And emotional factors, like depression and poor body image, can influence sexuality as well.
Men who take medications for Parkinson’s disease might develop premature ejaculation (PE), according to a June 2018 study.
Undergoing prostate cancer treatment can leave men both physically and emotionally spent. Common approaches like surgery, radiotherapy, chemotherapy, and hormone therapy often have side effects, including problems with urinary and bowel function, sexual function, and fatigue. The stress of a cancer diagnosis and feeling unwell, along with concerns about meeting obligations and planning for the future, may be overwhelming.
Obese men who have weight loss surgery might see their testosterone levels – and their sex drive – improve in a month, according to new research.
It’s not unusual for obese men to have low testosterone (also called hypogonadism).
For cervical cancer survivors, it can be difficult to adjust to changes in sexuality. Pain, poor lubrication, and anxiety are common issues, and it takes time to feel comfortable with sex again. For some women, the situation causes great distress. In fact, a recent study published in the journal Psycho-Oncology estimates that about a third of cervical cancer survivors feel sexual distress.
Is there an expert I can talk with - and bring into the conversation now, rather than after my treatments?
How can I be proactive in preserving my sex life or fertility?
What will the chemo/radiation/surgery do to parts of my body that have nothing to do with the cancer?
For people with gender dysphoria, transitioning from one’s birth gender to their desired gender can be a big step. It can involve hormonal treatment as well as surgery. Some professionals recommend a mental health screening and psychotherapy beforehand as part of the process. But is that really necessary?
Women’s orgasms might be influenced by a type of sexism called “benevolent sexism,” suggests a recent study in the Archives of Sexual Behavior.
Recent research suggests that older men on intermittent androgen deprivation therapy (ADT) for prostate cancer are at higher risk for certain adverse events.
Testosterone replacement therapy (TRT) doesn’t appear to cause or worsen lower urinary tract symptoms (LUTS) or an enlarged prostate, according to a review of past research.
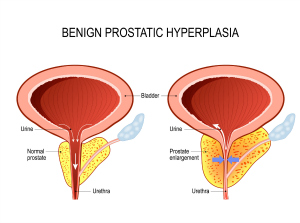
An enlarged prostate – also called benign prostatic hyperplasia (BPH) – is common as men get older. In fact, about half of men in their fifties have an enlarged prostate.
The condition is called postcoital dysphoria (PCD) and it’s not widely understood. Women with PCD may feel depressed, anxious, or argumentative, even if they enjoyed the sexual encounter.
The “general cosmetic appearance” of a man’s penis is important to women, according to new research published in The Journal of Sexual Medicine.
A painkiller called tramadol may help men with premature ejaculation (PE) “last” longer during vaginal intercourse, according to a new study.
Recreational use of amphetamines is associated with higher rates of erectile dysfunction (ED), according to a recent report in The Journal of Sexual Medicine.
Trichomonas vaginalis, a common sexually-transmitted parasite, could be involved with the development of prostate cancer, according to research published last year.
Men who feel good about their genitals tend to have less sexual anxiety, according to a new study of military personnel.
Many men with borderline low testosterone also have symptoms of depression, according to researchers from George Washington University.
Their study involved 200 men with borderline low testosterone, defined as total testosterone levels between 200 and 350 ng/dl.
What do sex addicts and people with gambling disorder have in common? A team of scientists from Spain recently looked at the similarities and differences between the two groups.
For some of us, taking care of our cancer patients involves the physical care. We might recommend surgery for our prostate cancer patients. Or we might order a certain chemotherapy regimen for a woman with ovarian cancer. Of course, we know that their mental health is extremely important, but we tend to focus on our area of expertise.
New research suggests that fathers-to-be experience declines in certain hormones when their partners are expecting a baby.
Hormonal changes are expected in pregnant women. But scientists from University of Michigan wanted to take a closer look at what changes men go through during their partner’s pregnancy.
For some women, a man’s premature ejaculation (PE) interferes with sexual satisfaction.
You may also be interested in...
Other Popular Articles

What Is the Average Penis Size?
If you have ever wondered how your penis compares to others in terms of size, you are not alone. Many men are curious to know how their penises stack up compared to the average. Unfortunately, general curiosity can sometimes give way to full-on obsession and anxiety about penis size. This can be an unhealthy and often unnecessary fixation, especially because most men who think their penises are too small have perfectly normal-sized penises.

What Is Jelqing, and Does It Actually Work?
The term “jelqing” refers to a set of penis stretching exercises that some believe can make the penis bigger. Although the practice has gained attention and popularity in blogs and internet forums in recent years, there is no scientific evidence that it is an effective way to permanently increase the size of one’s penis. In fact, in some cases, jelqing may actually cause damage to the penis, so it is a good idea to get all the facts before setting off to try it.

What Is Sensate Focus and How Does It Work?
Sensate focus is a technique used to improve intimacy and communication between partners around sex, reduce sexual performance anxiety, and shift away from ingrained, goal-oriented sexual patterns that may not be serving a couple.

Can Sex Reduce Menstrual Cramps?
The SMSNA periodically receives and publishes ‘guest editorials.’ The current article was submitted by Mia Barnes, a freelance writer and researcher who specializes in women's health, wellness, and healthy living. She is the Founder and Editor-in-Chief of Body+Mind Magazine.
Having sex while you experience menstrual cramps is healthy and can provide significant benefits. While it might not be the first activity that comes to mind when your PMS or period cramping begins, many people enjoy sex to reduce menstrual cramps, experience increased pleasure and benefit from other advantages. Learn more about having sex while menstrual cramps are happening and how it can help your body.

How Long Does It Take the Average Man to Ejaculate?
On average, it takes a man between 5 to 7 minutes to orgasm and ejaculate during sexual intercourse.

Can Sex Throw off Your Vaginal pH Balance?
The SMSNA periodically receives and publishes ‘guest editorials.’ The current article was submitted by Mia Barnes, a freelance writer and researcher who specializes in women's health, wellness, and healthy living. She is the Founder and Editor-in-Chief of Body+Mind Magazine.
Your vagina is a pretty powerful organ. It is a pathway for menstrual blood and babies. It also is a main player in sexual intercourse. You might hear about your vagina’s pH and worry that yours is at risk. Here’s what to know about vaginal pH, including the impacts sex could have.
You are prohibited from using or uploading content you accessed through this website into external applications, bots, software, or websites, including those using artificial intelligence technologies and infrastructure, including deep learning, machine learning and large language models and generative AI.






































































































.jpg)






.jpg)


.jpg)

.jpg)